Decoding the Mysteries: Does an MRI Show Nerve Damage?

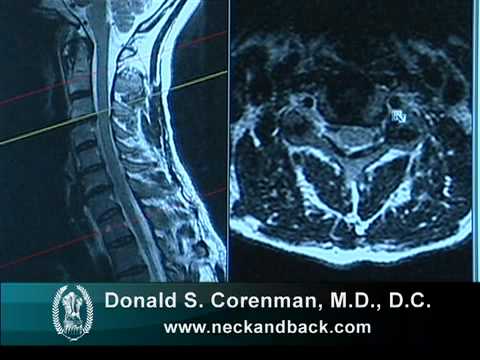
Does an MRI Show Nerve Damage? Magnetic Resonance Imaging (MRI) has evolved as a game-changing diagnostic technology, providing precise insights into the internal structures of the body. One frequently asked topic is whether an MRI can accurately detect nerve damage.
In this blog post, we’ll delve into the complexities of MRIs, investigating their potential to detect nerve damage. Understanding the complexities of this diagnostic procedure is critical for both individuals seeking solutions to nerve-related concerns and healthcare professionals seeking reliable diagnoses.
Let us solve the riddles and acquire insights into how MRIs can detect nerve injury.
The Power of MRI in Medical Imaging
The ability of MRI to acquire detailed images of inside structures makes it a powerful tool in medical diagnostics.
How MRIs Work:
Magnetic Resonance Imaging Imaging creates comprehensive cross-sectional images of the body’s internal architecture using powerful magnets and radio waves.
MRIs, unlike X-rays and CT scans, do not employ ionizing radiation. Instead, they generate images by using the magnetic characteristics of atoms within the body.
Nerves can be seen on MRI scans since they are part of the body’s complicated network. While MRIs excel at obtaining pictures of soft tissues such as muscles and nerves, diagnosing nerve injury requires thorough image processing.
Can MRIs Detect Nerve Damage?:
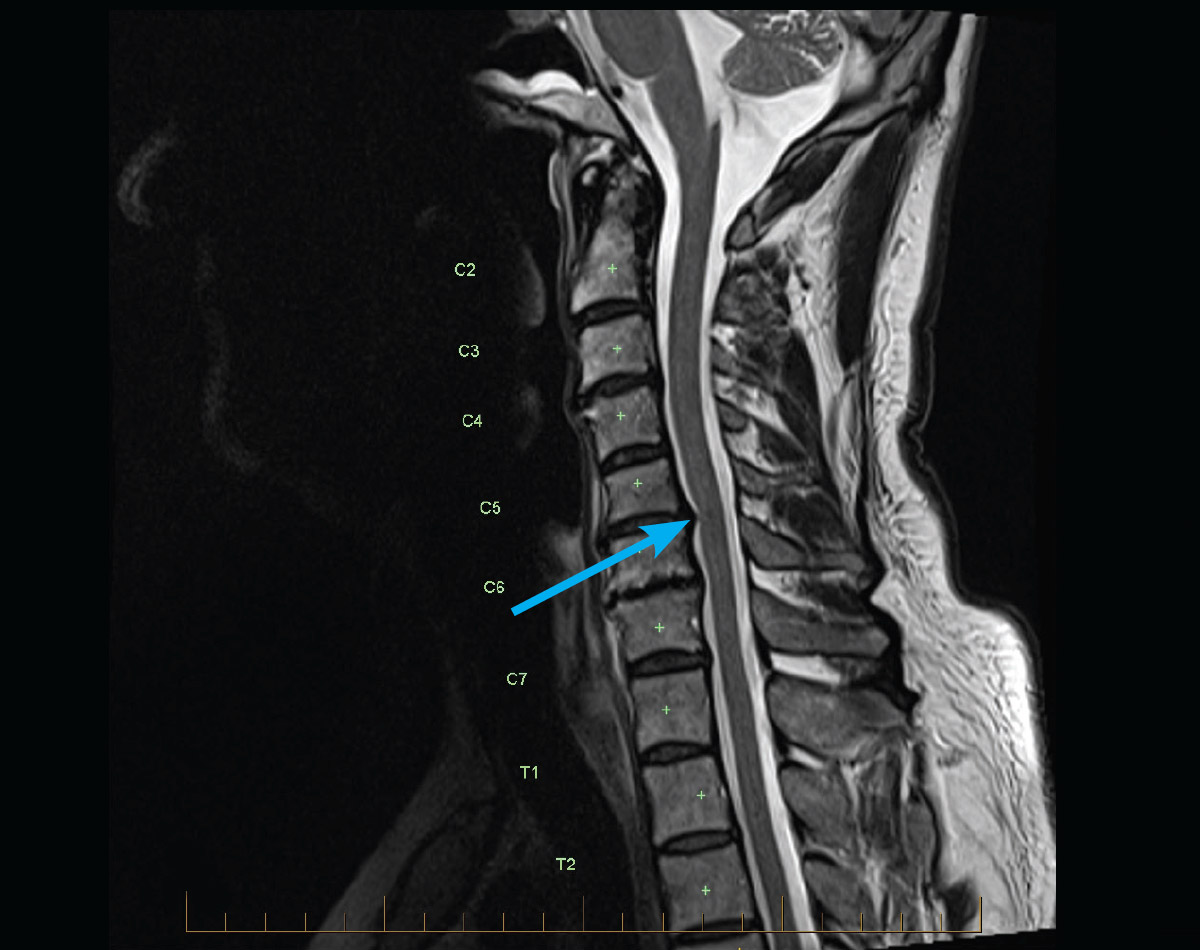
Yes, MRIs can detect nerve injury, but the technique is complicated. Nerve injury can appear in a variety of ways, and the amount to which it is evident on an MRI is determined by factors such as the form of the damage and the imaging sequences utilized.
- Soft Tissue Visualization: MRIs excel at imaging soft tissues, especially nerves. They can visualize the spinal cord, nerve roots, and peripheral nerves in great detail.
- Compression Detection: MRIs are especially useful in detecting conditions that cause nerve compression. Herniated discs and bone spurs, for example, can compress nerves and are frequently seen on MRI scans.
- Evaluation of Swelling or Inflammation: Swelling or inflammation may accompany nerve injury. MRIs can detect these alterations, providing information about the nerves’ general health.
- Tumor or Lesion Evaluation: MRIs can also detect abnormal growths or lesions affecting nerves. This includes malignancies that impact the peripheral nerves as well as disorders such as neuromas.
- Techniques for Functional MRI: In addition to classic structural imaging, emerging techniques such as functional MRI (fMRI) can provide information regarding the functioning condition of nerves.
While MRIs are strong diagnostic tools, they may not detect all types of nerve injury. Certain types of injury, particularly those involving tiny nerve fibers, may be difficult to detect on typical MRI scans.
Limitations and Considerations:
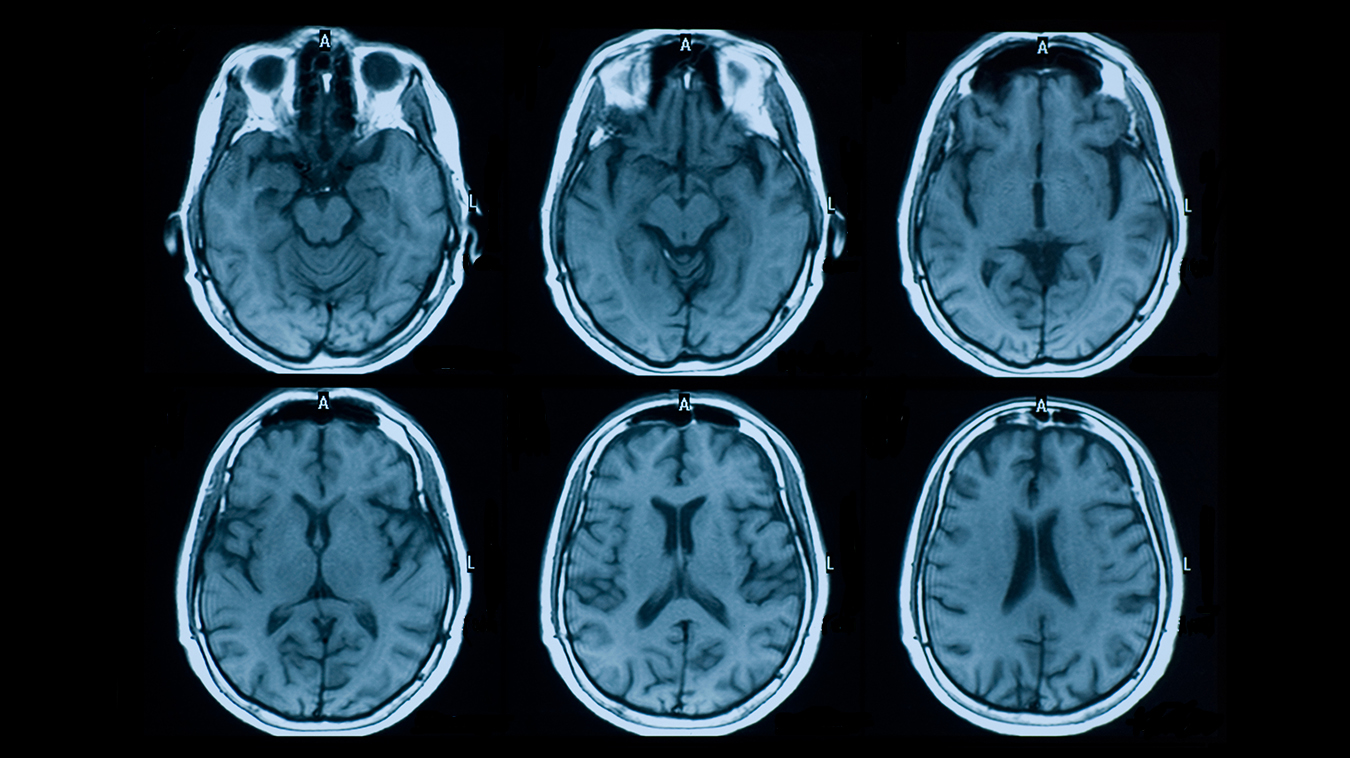
Despite its strengths, an MRI has limitations in terms of what it can disclose regarding nerve damage:
- Microscopic Nerve Damage: On normal MRI scans, small or microscopic nerve damage may not be visible.
- Functional Changes: While structural changes can be seen, functional changes within nerves may be missed unless specific procedures are used.
- Acute vs. Chronic Damage: On MRI, acute nerve damage, such as that produced by trauma, is generally more evident than chronic, progressive damage.
- Clinical Correlation: For a complete assessment, MRI findings must be correlated with clinical complaints and other diagnostic testing.
Individual characteristics such as the patient’s ability to remain still during the scan can have an impact on image quality.
FAQ About Does an MRI Show Nerve Damage?
Q1: Can an MRI definitively diagnose nerve damage?
A1: While MRIs are effective instruments for viewing soft tissues, including nerves, they may not be able to definitively diagnose all types of nerve injury.
Interpretation of MRI data frequently necessitates linkage with clinical complaints, and other testing may be required for a complete diagnosis.
Q2: What types of nerve damage can an MRI detect?
A2: MRIs are useful in diagnosing many types of nerve damage, such as compression caused by disorders such as herniated discs, anomalies producing inflammation or swelling, cancers affecting nerves, and lesions such as neuromas.
However, microscopic damage or certain forms of small fiber neuropathies may be more difficult to detect.
Q3: Are there specific MRI techniques for assessing nerve function?
A3: Emerging techniques, such as functional MRI (fMRI), can give information about the functional status of nerves in addition to classic structural imaging.
These approaches are currently in the early stages of development and may not be generally available for all therapeutic settings.
Q4: Can an MRI show chronic nerve damage?
A4: MRIs can detect chronic nerve injury, however the degree of visibility may vary depending on the nature of the damage. Traumatic nerve damage, for example, is generally more evident on MRI than slow, chronic damage.
Q5: Are there limitations to what an MRI can reveal about nerve damage?
A5: Yes, there are constraints. Microscopic nerve injury may be missed by MRIs, and functional changes inside nerves may necessitate specialist procedures.
A full examination requires clinical connection with symptoms as well as the use of additional diagnostic instruments.
Q6: Can an MRI detect nerve damage throughout the body?
A6: MRIs can identify nerve damage all across the body. They are frequently used to evaluate the spinal cord, nerve roots, and peripheral nerves. The imaging sequences utilized can be adjusted to specific parts of the body.
Q7: Is an MRI the only diagnostic tool for assessing nerve damage?
A7: No, an MRI is one of numerous diagnostic methods available for evaluating nerve injury.
In addition to MRI findings, clinical evaluation, nerve conduction investigations, electromyography (EMG), and other procedures may be utilized to offer a thorough assessment.
Q8: How long does an MRI for nerve damage take, and is it painful?
A8: The length of an MRI for nerve injury is determined on the exact area being studied. Although the operation is not normally uncomfortable, some individuals may experience discomfort as a result of extended posture.
It is critical to express any concerns or discomfort to the MRI technologist.
Q9: Can an MRI detect nerve damage caused by carpal tunnel syndrome?
A9: An MRI can reveal nerve damage caused by disorders like carpal tunnel syndrome. It can indicate structural abnormalities, inflammation, or nerve compression in the affected area.
Q10: Are there any risks associated with undergoing an MRI for nerve damage?
A10: MRIs are generally thought to be safe. They don’t use ionizing radiation. Individuals with specific medical disorders or metal implants, on the other hand, should notify the MRI technologist because there may be safety concerns.
Communication and, if necessary, sedative options can be used to treat claustrophobia or anxiety.
Conclusion:
Finally, MRIs are effective instruments for detecting and assessing nerve injury. They are particularly skilled at seeing soft tissues, detecting compression, and evaluating structural anomalies that may impact nerves.
The interpretation of MRI findings, on the other hand, necessitates a detailed understanding, and clinical linkage with a patient’s symptoms is critical. While MRIs can provide useful information, they may not catch all facet of nerve injury, particularly at the microscopic level.
As technology progresses, the use of functional MRI techniques and other developments may improve our ability to detect and comprehend nerve injury in greater depth.
For the time being, MRIs remain an important part of the diagnostic process, providing a thorough look at the complex topography of the human nervous system.
- Your Ultimate Guide to Travel Insurance for Adventure Sports
- A Guide to Renters Insurance for Pet Owners: Pet-Proof Your Policy
- Safeguard Your Future: Understanding Identity Theft Insurance
- Safeguard Your Event: Understanding Event Cancellation Insurance
- Everything You Need to Know About Critical Illness Insurance Riders
- Home Equity Loans vs. HELOCs: Which is Right for You?